My first two children were born by caesarean after long labours and foetal distress, and there was no skin-to-skin contact straight after birth – it was impersonal, like a business transaction. So when I discovered I was pregnant for a third time, I hoped to be able to have a natural vaginal birth.
Once my morning sickness had eased at about week 15, my pregnancy progressed well. I felt healthy and continued to exercise until 35 weeks.
Although my preference was for a vaginal birth after caesarean (VBAC), I was realistic, so researched different types of caesareans and discovered ‘maternal caesarean’, where a mum participates in a surgical delivery by lifting her baby out of her tummy.
Via Facebook, I found a couple of mothers interstate who had delivered this way at different hospitals within a week of each other, and they gave me more information about the procedure. I discussed this idea with my private midwife, who was supportive.
At about 33 weeks I contacted the obstetrician in charge at my local hospital, who explained it would be up to my care provider to make a decision. So I talked to my hospital obstetrician.
Although the procedure hadn’t been done at this hospital, he had watched one when he was training interstate and would consider doing it if the surgery was planned, not emergency, and there was no increased risk of infection. So I wrote up a birth plan which clearly stated my wishes – VBAC or, if unable, maternal caesarean.
At about 36 weeks pre labour began – I lost the mucous plug, had a bloody show, irregular and long contractions and started dilating. This was accompanied by back pain and horrendous pelvic pressure – to the extent I was struggling to walk, and felt like I needed to push to counteract the pressure. I was in agony.
After almost two weeks of this pain, my midwife and I agreed I needed monitoring to ensure my baby was okay and to find out what could be delaying the onset of established labour, as I was 6cm dilated, before we considered induction.
We both thought my body was protecting itself or the baby by not progressing with labour.
My obstetrician happened to be on duty when I went to the hospital for monitoring. My baby was fine, and my waters were bulging, which could explain the pressure in my pelvis. While my obstetrician was happy to support me to VBAC and, if I wished, would break my waters to encourage natural labour, he also thought my body might be protecting the baby.
Considering the pain was getting worse each day, I had two young children at home who needed their mummy, I was technically in labour and more than halfway dilated, my obstetrician offered to do a caesarean delivery.
He didn’t usually perform surgical deliveries so early in labour, but given my body’s state of readiness and my increasing disheartedness, he felt comfortable in doing so. I reminded him of our chat about maternal caesareans and he agreed to this, as long it was done that day while he was on duty.
So I took my older children home, gave them lunch and watched a movie with them, then returned to hospital with my midwife and friend. Meanwhile the obstetrician had briefed the theatre team and explained my wishes.
Mid-afternoon I was wheeled into theatre. It was so different to my previous experience when I was in agony and everything was a blur. This time it was my choice, and I was at peace with the decision.
The theatre team prepped me and inserted the spinal block while I held hands with one of the team. His kindness letting me squeeze his hand meant so much to me – it made me feel safe. While the anaesthetic took effect I was scrubbed, then forbidden to move my hands.
My midwife arrived and we chatted, then I heard someone say, “Let’s get her gloved”, and I knew the birth would be soon. I was told not to move my hands until told to reach down.
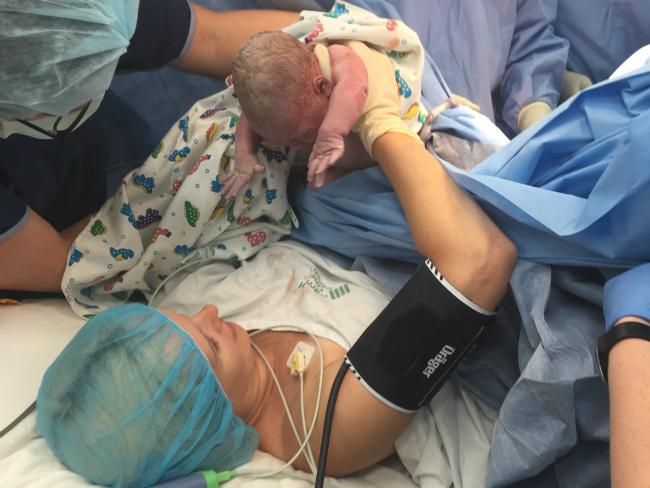
Not long after the drapes were lowered. I saw my baby’s head come out, heard a little cry and in the same moment was told to reach for her. As I held her little body under her arms and pulled her out I could feel myself swell with tears.
I was in awe.
I got to see all of her as I lifted her from my body into the air and placed her safely on my chest, where she immediately settled.
My little girl was here. I cried – and I think I saw tears in everyone’s eyes. It was a beautiful moment.
My obstetrician popped his head over and explained that Emma wouldn’t have been born naturally had I tried to birth – she was stuck on my pubic bone and had a mark across her head where she sat.
I would have been in for a painful labour that would have ended in another emergency caesarean. Then he said he was going to stitch me up while I enjoyed skin-to-skin contact with my newborn.
I was able to just stare at her and feel her on me, she was so warm. She snuggled up into my chin then started rooting around and attached for a breastfeed.
The theatre team were amazed to see her feeding so soon. Even in recovery she never left me; for hours on end we just snuggled into each other. My older children arrived and were smitten with their little baby sister.
Finally I was whole.
The arrival of Emma was a beautiful, healing birth for me – but I would never have known about if I hadn’t educated myself about my rights to birth how I wanted.
I pushed for my right to have a VBAC and then a maternal caesarean. While I compromised on my natural birth I still felt empowered. I’m so grateful for the care of my midwife and obstetrician and the hospital staff, and I really hope that other mums are able to have the same wonderful and life-changing experience.