Unlike my previous pregnancies, my seventh pregnancy was troublesome right from the beginning. At seven weeks I lost one of the twins I was carrying. From that point onwards, I experienced 10 bleeds, and each time I had to go to hospital to check if I was still carrying a live baby.
After a bleed at 22 weeks, I was diagnosed with placenta praevia [where the placenta implants at the bottom of the uterus, covering the cervix and preventing a vaginal delivery]. A caesarean was scheduled for 37 weeks, but since I could bleed at any time and would need to be rushed into theatre, I was told to take it easy and not leave the local area.
My doctors discussed the possibility I had placenta accreta [when the placenta becomes embedded in the uterine wall] but weren’t convinced as it wasn’t clear on the ultrasound. After taking it quietly, at 36 weeks I was sitting at home with my six children when I suddenly felt a gush of fluid. I had a split second of dread and immediately knew what was happening. In the bathroom I discovered blood pouring out and called for the kids to bring me the phone, so I could call for an ambulance. Then I messaged my husband via Facebook (“Help. Come home now. Bleeding.”) and a friend to come quickly.
The paramedics arrived within 10 minutes, put a drip in me and rushed me to hospital as blood continued to flow. Ben, my husband, got home just a few minutes before the ambulance took off, so followed in his car. Contractions began during the journey, so the paramedics rang to warn the hospital, and an operating theatre was prepared for me. Ben arrived as I was being wheeled into theatre and we had a few seconds together. During the pregnancy we had discussed how serious my condition could become, so I had told my husband a couple of times what my wishes were if the worst happened. This was the moment when those conversations became more real.
Life-saving surgery
The operating theatre was filled with busy medical staff. I tried to remain calm while needles were inserted into my body, questions were asked and a midwife checked for the baby’s heartbeat with a Doppler. She couldn’t find it until I told her the baby was breech, and everyone seemed to breathe easy again. It was all systems go with one doctor asking me questions, another waxing me and a third doing an internal examination to make sure the placenta wasn’t coming out. At this point I realised I’d probably need a hysterectomy.
My last memory was asking the date so I would know when my baby was born. Little did I know how critical the situation was and just being able to see my baby was uncertain. As I was being put under a general anaesthetic, a nurse had to press her hand into my neck to stop me choking on the food in my stomach. I felt like I was being strangled but the only way to get through it was to breathe deeply and put myself to sleep faster.
All the action happened while I was unconscious. My little girl, Marcella, was delivered soon after the anaesthetic took effect. She had an Apgar score of four, but quickly improved and was moved to recovery in the neonatal intensive care unit (NICU). Marcella weighed 3.2kg and was perfect in every way, entirely unaware – as newborns are – of the chaos surrounding her.
Then the work to save my life started. During surgery doctors discovered I had the worst type of placenta accreta, percreta, when the placenta grows through the uterus and the cervix, attaching to the urethra, bladder and blood vessels. There was so much blood loss it was hard for doctors to know where the placenta finished and I began.
After nine hours of surgery, Ben was sent home. He managed to get all the children, who’d been staying with friends, into bed by 11pm. But he returned to the hospital just after 1am when informed my condition had worsened.
All up, I required 23 hours of surgery, a full hysterectomy and repairs to my bladder and urethra. I spent five days on life support and had a massive blood transfusion. NICU staff cared for Marcella and told Ben to take pictures of all her ‘firsts’ – first bath, cuddle and so on – for me to treasure if I survived. The medical team said they were “holding me here on earth by my heels”.
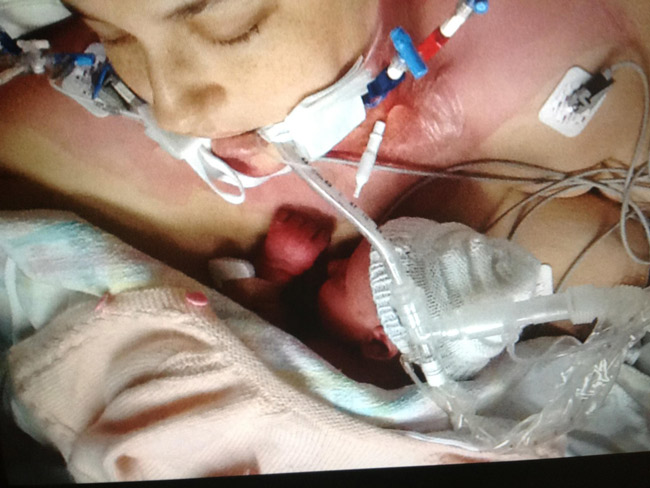
I finally got to meet my baby on day six of her life, but could only hold her for a few minutes because I was so weak. This was actually her third visit to me – unsure I would make it, the NICU nurses brought her to my room on day two and put her skin-to-skin on my chest, hoping this would encourage my will to survive. I do remember being in a sleep-like state and lifting my head to smell Marcella and rub my chin on her little head. A nurse later told me how I had instantly responded when Marcella was placed on my chest, and I believe this was a contributing moment in my fight for survival.
After four weeks in hospital I was finally strong enough to go home. Recovery was prolonged, but I’m now back to my full physical strength, albeit with some life-long complications: I’ve lost some kidney function, plus feeling in the top of my right leg and stomach from my belly button downwards. I also have optical nerve damage.
A rare condition, placenta accreta has become more common – I believe due to the increase in caesareans plus some contraceptive methods that can scar the uterus. I’m now president of the Australian chapter of the Hope for Accreta Foundation and am working with the Australian Red Cross to organise a global blood drive for early next January to increase blood donations. Helping other families in this way has been a huge part of my healing from this traumatic event.

Placenta Accreta: The facts
This serious but rare obstetric condition occurs in about one in 2500 pregnancies (0.04%). It’s difficult to diagnose, but risk factors include previous caesarean section and increasing maternal age. Pregnant women with placenta praevia and previous uterine surgery are at high risk, particularly if they have had two or more caesareans. An ultrasound may diagnose the condition, showing the placenta to be growing into the muscle of the uterus. Placenta accreta prevents the placenta from separating properly from the uterus. It may cause bleeding during pregnancy, but more often following delivery. Heavy bleeding may lead to a blood transfusion and, very rarely, a hysterectomy.


