It was a chance discovery by all accounts. Fresh out of university after completing a science degree, Dharmica Mistry began working as a lab technician at a small start- up company looking at the association between breast cancer and scalp hair.
“One day, I used my own hair as a control and found that it gave the same pattern as though I had breast cancer,” recalls Dr Mistry. “There was no reason to suspect that I had breast cancer, so my supervisor, Dr Peter French, quizzed me as to what I had done to my hair. ‘Nothing’, I replied, before suddenly remembering that I had sprayed it with olive oil to make it glisten.”

Scientist Dharmica Mistry. PHOTO: Nick Cubbin.
It was only then that Dr Mistry and Dr French realised what could be the biggest breakthrough in breast cancer detection – that lipids (oils that exist in the membranes of every cell in our body) were coming from the blood of breast cancer patients and being deposited in their hair.
Looking back, Dr Mistry says she would moisturise her long, black locks with oil every few months to help it shine. She is still astounded that a simple beauty trick helped her unearth a new way to detect breast cancer. “It was a very exciting finding,” she says. Her ground-breaking research earned her the title of 2015 Young Scientist of the Year and 2016 NSW Young Woman of the Year.
Born in England to Indian parents, Dr Mistry moved to Australia when she was just six. Her family settled in Sydney’s Sutherland Shire and Dr Mistry attended Oyster Bay Primary School and Gymea Technology High School, before completing a science degree at the University of Sydney. “I have amazing parents who have sacrificed so much so I could be given such a wonderful opportunity,” she says.
Now the Chief Scientist at BCAL Diagnostics, a company which she co-founded, Dr Mistry, 30, is determined to make the blood test accessible and affordable for all women. “My main drive and focus is to get this test out there to women around the world,” she says. “The test will be as simple as heading to your doctor for a blood test, as we do for many other regular check-ups, and the customer will have their blood taken through a pathology group.
The pathology laboratory will process the sample and send the results back to the customer’s doctor.”

Dr Mistry hopes to have the breast cancer blood test available by 2018. PHOTO: Nick Cubbin.
It sounds simple enough, but Dr Mistry acknowledges there is still much to do in her quest to have an accurate and non-invasive way to diagnose breast cancer for women of all ages.
“We expect to begin our clinical trials in 2017 and hope to have a test on the market by 2018-19,” she says.
Preliminary tests, however, are positive, showing 90 per cent accuracy with the test’s ability to identify early-stage invasive breast cancer. Currently, mammograms are the primary diagnostic tool in breast cancer detection for women over 50, but Dr Mistry says the test is not ideal.
“There is no doubt that the nationwide BreastScreen program saves lives by identifying the presence of cancer in a woman’s breast through routine screening using mammography, but it has a number of limitations, mainly limited accuracy for women under the age of 50 due to their high breast density,” she says. “Furthermore, only just over half of women over 50 are having their routine screening. The reasons for this low participation rate range from inconvenience of having to go to a central screening clinic to the uncomfortable nature of the examination.”
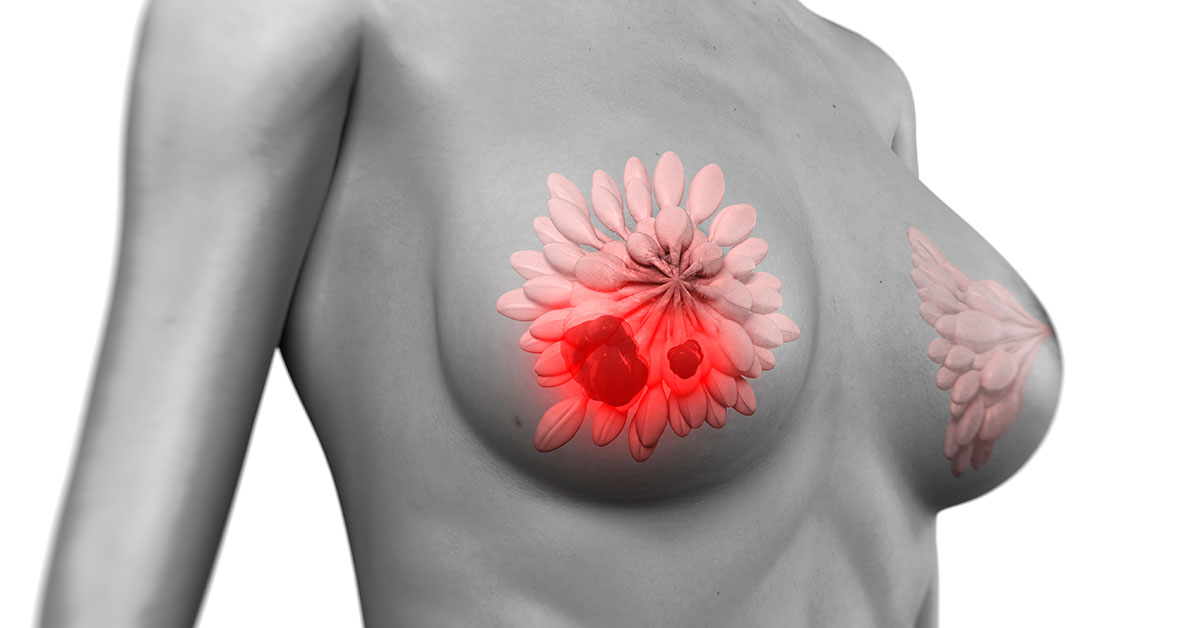
A computer generation of how breast cancer can grow deep under the breast tissue – making it hard to detect through self-examination. PHOTO: Getty.
Younger women, however, are reliant on self-examination. “I find it incredible that we have advanced so much in the world of medicine, yet the ‘best’ way to detect breast cancer in women under the age of 50 years old is still only by physical examination of the breast,” says Dr Mistry.
“By the time a lump is identified by feel, it can be quite advanced, meaning that the treatment options are limited, especially in younger women. We also have so many women under 50 who have a strong family history, but no reliable way to detect the disease early.
“Clearly, we need a more accurate screening tool that can be used for women of all ages more regularly and one which is more accessible to women in remote and rural areas worldwide.
“Mammography would still have a key place in breast cancer detection, but the hope is the BCAL blood test would assist in reaching women who currently can’t [due to age or surgery] or choose not to be routinely screened by mammography.
“A highly accurate blood test would revolutionise the way we screen for breast cancer, a disease that is so common and affects one in eight women.
A version of this story was originally printed in the October issue of The Australian Women’s Weekly.
WATCH: Inside Roxy Jacenko’s cancer removal operation


